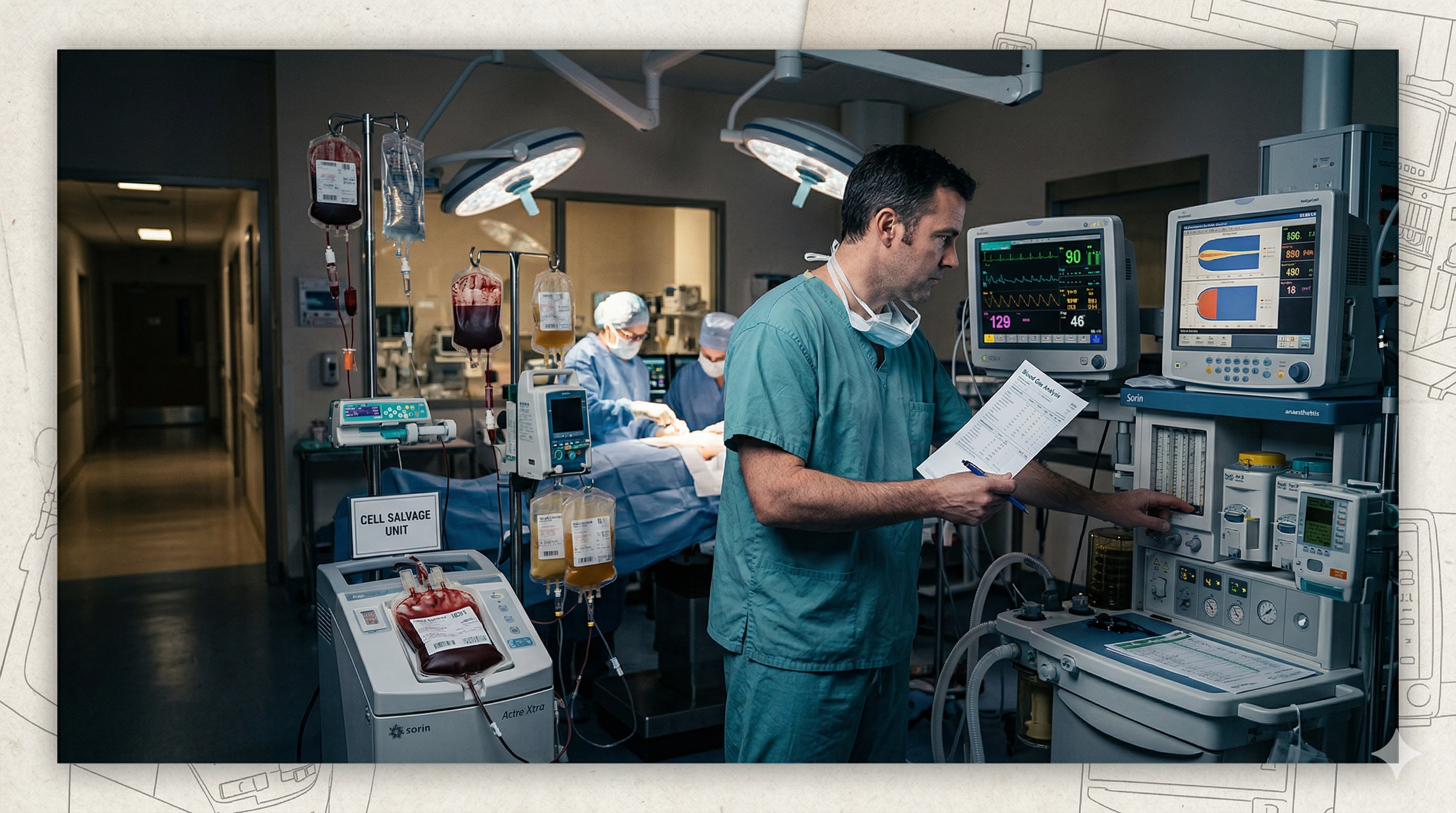
A patient presents for elective spinal revision surgery. She weighs 55 kilograms. Her total circulating blood volume is roughly 3.8 litres. Over the next twelve hours, she will lose more than twice that.
In a major public hospital, this scenario triggers a massive transfusion protocol with a dedicated team. A haematology registrar coordinates blood products. A second anaesthetist steps in. Nursing staff rotate through.
In private practice, none of that exists. The anaesthetist managing that case is alone.
What Massive Transfusion Actually Means
The Australian Red Cross Lifeblood guidelines define critical bleeding as haemorrhage requiring five or more units of packed red blood cells within four hours, or bleeding in a critical anatomical area such as the spine. At 30 to 40 per cent blood volume loss (roughly 1,500 to 2,000 millilitres in an average adult), red cell transfusion becomes necessary. Beyond 40 per cent, the situation is immediately life-threatening.
These thresholds sound clinical and orderly on paper. In practice, they arrive without announcement. A spinal osteotomy that has been proceeding methodically for six hours encounters a vascular plexus. Bleeding that was manageable becomes torrential. The transition from routine to critical can happen in minutes.
The Private Practice Reality
Public hospitals have systems designed for this. The blood bank is downstairs. The massive haemorrhage protocol is a phone call. Reinforcements exist.
Private hospitals have blood available, but the depth of supply is different. A public trauma centre might hold hundreds of units of packed cells on site. A private surgical hospital holds enough for routine lists. When a case consumes the entire platelet supply of a private facility, there is no overflow from a neighbouring ward. Fresh stock has to come from the blood bank, and that takes time.
The anaesthetist in this setting is managing the airway, maintaining anaesthesia, running the fluid resuscitation, ordering blood products, interpreting coagulation results, managing the cell salvage machine, communicating with the surgeon, and keeping an eye on the clock. All simultaneously. All alone.
This is not a failure of the private system. It is the reality of it. Complex surgery happens in private practice because patients and surgeons choose it. The anaesthetist who accepts these lists accepts the full weight of what they might become.
Blood Product Management Under Pressure
The principles of massive transfusion are well established. The Association of Anaesthetists recommends a ratio-based approach: red cells, fresh frozen plasma, and platelets delivered in balanced proportions. The Australian guidelines specify a minimum of four units of FFP and one adult unit of platelets for every eight units of red cells.
But ratios are a starting framework, not a recipe. During a twelve-hour case with ongoing blood loss, coagulation changes continuously. Fibrinogen drops. Platelets are consumed. Hypothermia and acidosis compound the coagulopathy. The anaesthetist is interpreting point-of-care tests in real time and adjusting the replacement strategy on the fly.
Fibrinogen management is particularly critical in prolonged haemorrhage. The threshold for concern is a level below 1 gram per litre. Cryoprecipitate is the standard replacement, but it takes time to thaw and prepare. In a fast-moving situation, every delay in fibrinogen replacement extends the window of coagulopathy and compounds the bleeding.
Cell salvage becomes essential. Collecting shed blood, washing and filtering it, and returning the patient's own red cells buys time and reduces the demand on banked products. But the machine needs someone to operate it. In a public hospital, a perfusionist or dedicated technician runs cell salvage. In private, the anaesthetist may be managing this alongside everything else, or relying on a scrub nurse who has had limited exposure to the equipment.
Acid-Base: The Quiet Indicator
Among anaesthetists, the state of a patient's acid-base balance at the end of a long, bloody case is the real marker of how well the resuscitation was managed. It is not glamorous. It does not make the surgical report. But it tells you whether oxygen delivery was maintained, whether the fluid strategy was right, whether the patient was adequately perfused through the worst of it.
A patient who loses ten litres of blood over twelve hours and arrives in intensive care with a normal acid-base profile did not get there by accident. That result reflects thousands of micro-decisions: when to transfuse, what to transfuse, how fast, what temperature, what the lactate was doing an hour ago versus now. It reflects an anaesthetist who was ahead of the bleeding rather than chasing it.
An intensivist receiving that patient might reasonably expect metabolic derangement. When the blood gas comes back normal, it is worth pausing on what that actually represents.
What This Means for Training
Anaesthesia registrars in Australia train primarily in public hospitals. They see massive transfusions in the context of trauma teams, haematology support, and senior cover a phone call away. This is appropriate for training. But it can create a gap.
The registrar who transitions to private practice may encounter their first truly solo massive haemorrhage years into their career. The physiology is the same. The protocols are the same. But the operational reality is completely different. There is no cavalry. The decision to call for help has to be made early, because help may take thirty minutes to arrive, not three.
The experienced private anaesthetist develops a different situational awareness. They think further ahead. They order products before they are needed rather than when they become urgent. They establish a relationship with the blood bank at the start of any case that carries significant bleeding risk, not when the bleeding starts. They have already counted the platelets in the fridge.
None of this is taught explicitly. It is learned through exposure. And occasionally through the controlled terror of a case that tests everything you thought you knew.
The Weight of Solo Practice
There is a particular kind of fatigue that follows a twelve-hour case with major blood loss managed alone. It is not just physical tiredness. It is the cumulative weight of sustained high-stakes decision-making without the relief of shared responsibility.
Surgeons have registrars to hold retractors, to share the technical burden. Anaesthesia in private practice is frequently a solo discipline. The anaesthetist starts the case and finishes the case. There is no handover, no shift change, no fresh set of eyes. This is accepted as normal, and mostly it is fine. But on the days when a routine list becomes a critical event, the isolation of the role becomes very real.
The patient recovers. The surgeon is satisfied. The intensivist is impressed. The anaesthetist drives home.
Dr Adam Hill is a specialist anaesthetist (FANZCA) practising in Sydney and regional NSW, with particular expertise in complex spinal, neurosurgery, and obstetric anaesthesia. He also flies his own aircraft to deliver specialist services to regional communities.