The Invisible Doctor: Why Patients Rarely Know What Their Anaesthetist Did
By Dr Adam Hill, Specialist Anaesthetist (FANZCA), Sydney, Australia
After most surgeries, patients remember the name of their surgeon. They remember the ward nurses who looked after them. They may remember the receptionist who booked them in. The anaesthetist, more often than not, is a blur. A friendly face at the head of the bed, a brief conversation before the operation, and then nothing until recovery.
This is not a failing of memory. It is the nature of the specialty. Anaesthetists do most of their work while the patient is either unconscious or focused entirely on something else. They operate behind a drape, out of the patient's line of sight, managing the systems that keep a person alive while someone else performs the surgery. The Helsinki Declaration on Patient Safety in Anaesthesiology frames this work as the foundation of perioperative safety, even when it is not visible to the patient [1]. When everything goes well, there is nothing dramatic for the patient to remember. That is precisely the point.
More Than "Putting You to Sleep"
The most common description patients give of anaesthesia is that the doctor "put them to sleep." It is an understandable shorthand, but it misses about 95 per cent of the job. Inducing anaesthesia (the part where the patient loses consciousness) takes a few minutes at most. The remaining hours are spent managing the patient's physiology through what is, by any measure, a controlled physiological crisis.
Surgery involves tissue injury, blood loss, fluid shifts, changes in body temperature, alterations in heart rate and blood pressure, and the constant potential for unexpected complications. The anaesthetist monitors and manages all of this in real time, adjusting medications, fluids, and ventilation breath by breath.
In a typical operation, the anaesthetist is responsible for:
Airway management. Once a patient is under general anaesthesia, they cannot breathe independently. The anaesthetist secures the airway (usually with an endotracheal tube or laryngeal mask) and controls ventilation for the entire procedure. In patients with difficult anatomy, previous surgery, or conditions affecting the spine or jaw, this alone can be the most technically demanding part of the case. The Fourth National Audit Project of the Royal College of Anaesthetists and the Difficult Airway Society identified airway events as a leading cause of major anaesthetic morbidity, with most adverse outcomes traced to failures of planning rather than failures of skill [2].
Cardiovascular stability. Blood pressure, heart rate, and cardiac output are continuously monitored and actively managed. Surgery triggers stress responses that alter circulation. Blood loss reduces the volume in the system. Anaesthetic drugs themselves affect the heart and blood vessels. Keeping these parameters within a safe range requires constant attention and intervention.
Blood management. Some operations involve significant blood loss. The anaesthetist monitors haemoglobin levels, coagulation, and acid-base balance, and coordinates transfusion of blood products when needed. In major cases (complex spinal surgery, trauma, major obstetric haemorrhage), this becomes a high-stakes exercise in real-time physiology, sometimes involving the replacement of the patient's entire blood volume. The Australian National Blood Authority's Patient Blood Management Guidelines describe the protocols and ratios that govern these decisions in critical bleeding [3].
Pain control. Managing pain during surgery is only part of the equation. The anaesthetist also plans and initiates the post-operative pain strategy before the patient wakes up. Regional nerve blocks, epidurals, patient-controlled analgesia devices, and multimodal medication regimens are all part of the anaesthetist's toolkit. The quality of pain management in the first 24 hours has a direct effect on recovery, mobility, and the patient's overall experience. The Enhanced Recovery After Surgery (ERAS) literature has consistently shown that multimodal analgesia, opioid-sparing techniques, and regional anaesthesia reduce length of stay and improve functional recovery across surgical specialties [4].
Temperature regulation. Body temperature drops under anaesthesia. Even a small reduction increases the risk of wound infection, delays clotting, and slows recovery. The landmark trial by Kurz, Sessler and Lenhardt demonstrated that maintaining intraoperative normothermia reduced surgical site infections threefold and shortened hospital stay [5]. The anaesthetist uses forced-air warming devices and warmed intravenous fluids to maintain normal temperature throughout the case.
Behind the Drape
In the operating theatre, a sterile drape separates the surgical field from the patient's head and upper body. The surgeon works on one side. The anaesthetist works on the other.
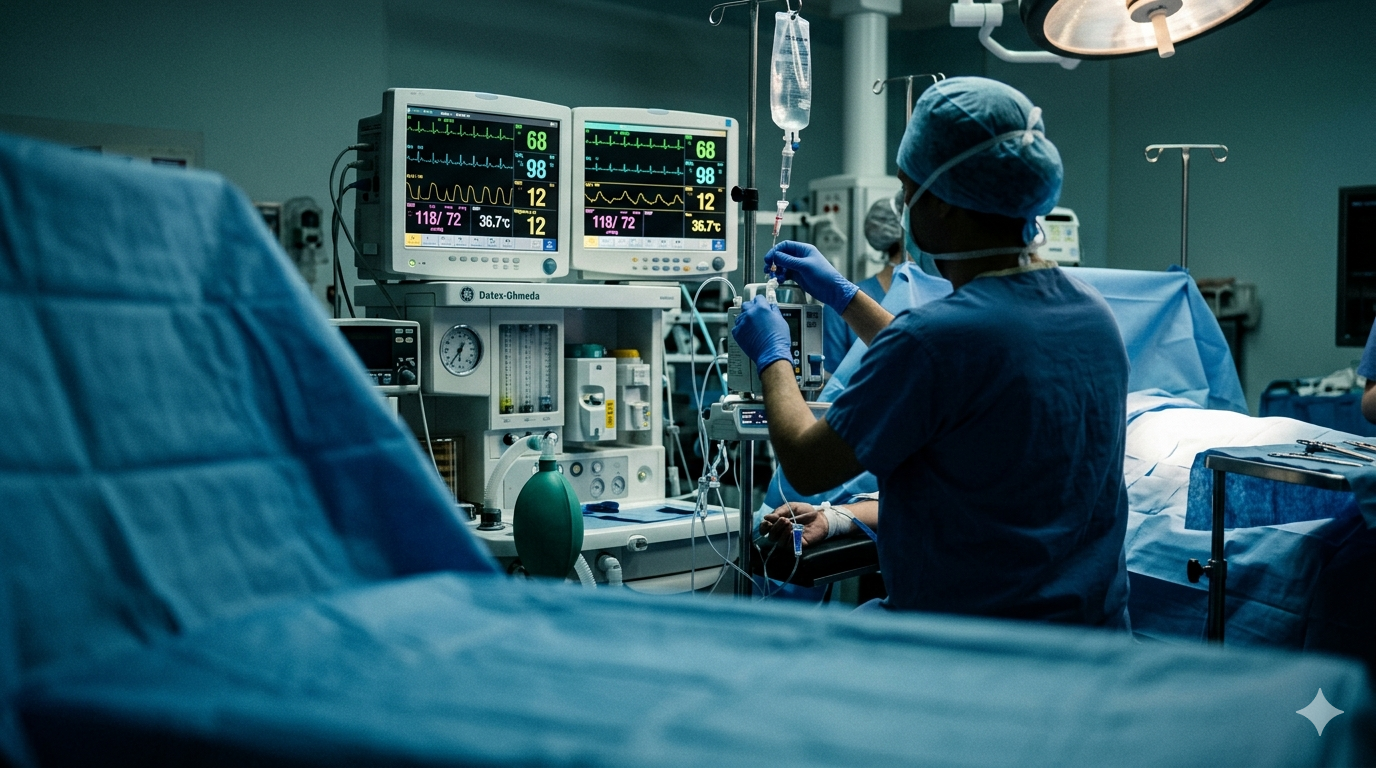
From the surgical side, the operation is visible and dramatic. Tissue is cut, structures are identified, implants are placed, wounds are closed. From the anaesthetist's side, the work is quieter but no less complex. A bank of monitors displays heart rhythm, oxygen saturation, blood pressure, exhaled carbon dioxide levels, anaesthetic gas concentrations, and temperature. Infusion pumps deliver precise doses of multiple drugs simultaneously. The anaesthetist is reading all of this information continuously, making adjustments that the surgical team and the patient will never see.
If the patient is awake (as in a caesarean section under spinal anaesthesia or certain orthopaedic procedures under regional block), the anaesthetist is also managing their comfort, anxiety, and awareness. Talking to a patient, keeping them calm, managing nausea, and adjusting medications while monitoring their physiology is a particular skill that sits at the intersection of clinical medicine and human connection.
When It Matters Most
The cases that illustrate the anaesthetist's role most clearly are the ones where things become complicated. A patient who bleeds more than expected. An airway that proves difficult to secure. A sudden change in heart rhythm. An unexpected allergic reaction to a medication.
In these moments, the anaesthetist is the doctor managing the crisis, often before anyone else in the theatre is aware there is a problem. The training for this is rigorous and specific: years of managing simulated and real emergencies, from cardiac arrest to anaphylaxis to massive haemorrhage. The goal is to respond quickly and effectively enough that the patient never knows how close the situation came to becoming serious.
In complex surgery (operations lasting many hours, involving significant blood loss, or performed on patients with multiple medical conditions), the anaesthetist's contribution is often the difference between a straightforward recovery and a prolonged stay in intensive care. The quality of intraoperative management directly affects post-operative outcomes. A meta-analysis of perioperative mortality in developed countries found that anaesthesia-attributable mortality has fallen below 1 in 100,000 cases in the modern era, an achievement built on continuous monitoring, structured handover, and the systematic management of physiological variables that the patient never sees [6].
The Personality of the Specialty
Anaesthesia tends to attract a certain kind of doctor. The specialty demands comfort with uncertainty, the ability to remain calm under pressure, and a willingness to work without recognition. There is no outpatient follow-up. No long-term relationship with the patient. The anaesthetist does their work, the patient recovers, and in most cases, that is the end of the interaction.
This suits some doctors very well. The satisfaction comes from the work itself: from keeping a patient safe through a difficult case, from managing a crisis that no one else noticed, from the quiet knowledge that the physiology was optimised and the pain was well controlled. It is a specialty built on the principle that the best outcome is the one where nothing appears to have gone wrong.
What Patients Can Do
If you are having surgery, your anaesthetist will meet you beforehand. This is a good opportunity to ask questions, mention any previous experiences with anaesthesia (good or bad), and discuss any concerns about pain management or nausea. The pre-operative conversation is not a formality. It directly informs the anaesthetic plan.
After surgery, if you had a good experience (you were comfortable, your pain was well managed, you felt safe), that is worth mentioning. A brief word to the nursing staff or a note to the hospital goes a long way in a specialty where direct patient feedback is rare.
The anaesthetist may be invisible during the operation. But the work they do is anything but.
References
- Mellin-Olsen J, Staender S, Whitaker DK, Smith AF. The Helsinki Declaration on Patient Safety in Anaesthesiology. Eur J Anaesthesiol. 2010;27(7):592-597.
- Cook TM, Woodall N, Frerk C; Fourth National Audit Project. Major complications of airway management in the United Kingdom: results of the Fourth National Audit Project of the Royal College of Anaesthetists and the Difficult Airway Society. Part 1: anaesthesia. Br J Anaesth. 2011;106(5):617-631.
- National Blood Authority. Patient Blood Management Guidelines: Module 1 — Critical Bleeding/Massive Transfusion. Canberra: National Blood Authority; 2011.
- Joshi GP, Kehlet H. Postoperative pain management in the era of ERAS: an overview. Best Pract Res Clin Anaesthesiol. 2019;33(3):259-267.
- Kurz A, Sessler DI, Lenhardt R. Perioperative normothermia to reduce the incidence of surgical-wound infection and shorten hospitalization. N Engl J Med. 1996;334(19):1209-1215.
- Bainbridge D, Martin J, Arango M, Cheng D. Perioperative and anaesthetic-related mortality in developed and developing countries: a systematic review and meta-analysis. Lancet. 2012;380(9847):1075-1081.